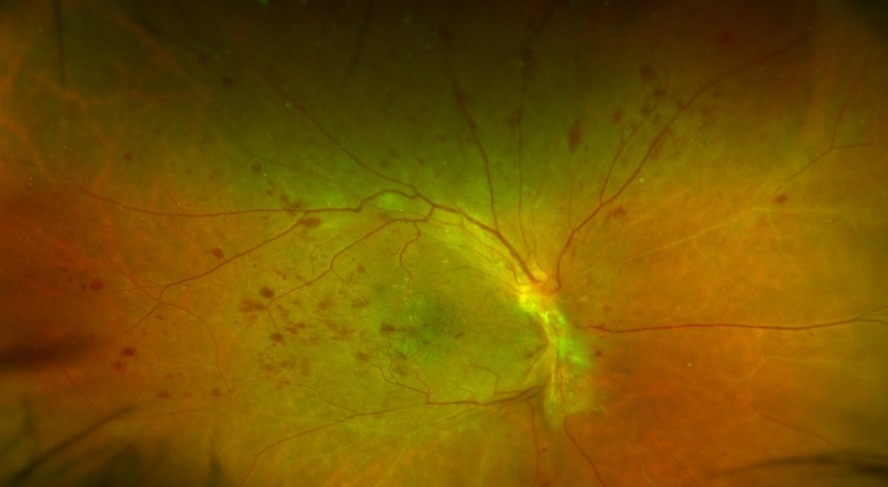
Diabetic Retinopathy
Diabetic retinopathy is a complication of diabetes mellitus and is one of the main causes of blindness in young and middle-aged adults. It occurs when diabetes damages the tiny blood vessels
Diabetic retinopathy does not cause symptoms or signs in the early stage. But over time it can lead to vision loss and even blindness.
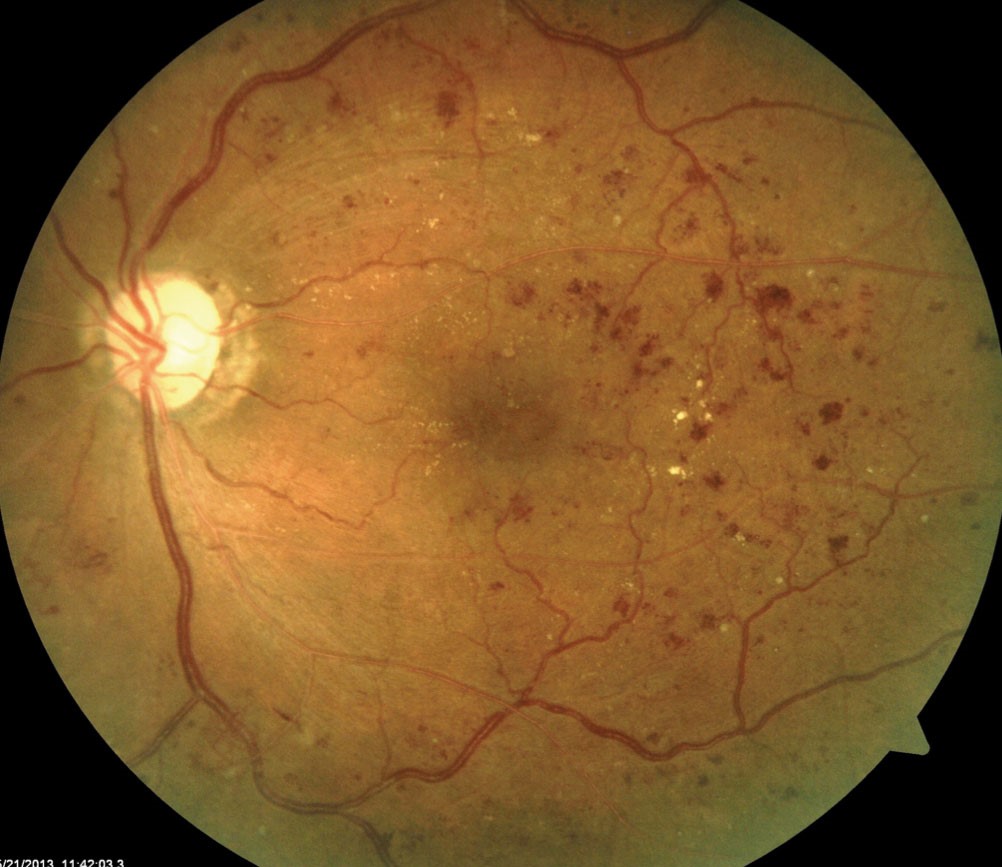
Diabetic Retinopathy with widespread bleeding of the retina in above photo.
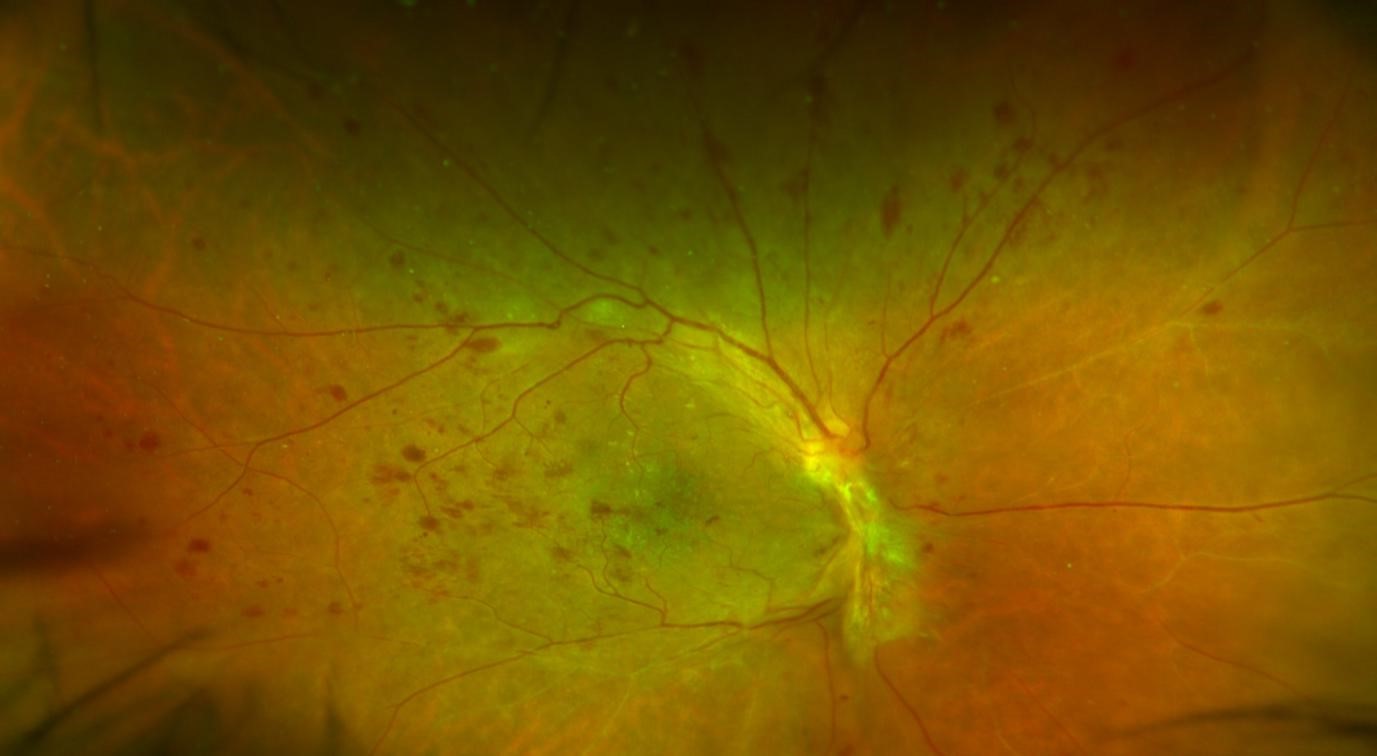
More severe diabetic Retinopathy with widespread bleeding and scarring / fibrosis of the retina in above photo.
What are the types of diabetic retinopathy?
Non-proliferative diabetic retinopathy, also known as background diabetic retinopathy, is the early stage of diabetic retinopathy and occurs when the small retina blood vessels become affected and begin to leak and bleed. At this stage, vision is usually not affected since mainly the peripheral retina is involved
Proliferative diabetic retinopathy is associated with a high risk of permanent loss of vision. There is growth of abnormal new blood vessels in the retina. These abnormal new vessels can rupture, causing significant bleeding and damaged retina and that will lead to loss of vision.
Scar tissues form and caused traction and retinal detachment. The abnormal blood vessels can grow on the iris and block fluid outflow from the eye. Neovascular glaucoma can develop with a risk of optic nerve damage and blindness.
The central retina can also be affected by diabetic macular oedema. In the severe stages of diabetic retinopathy, vessels in the centre of the retina leak fluid causing retinal swelling and loss of central vision.
Diabetic Retinopathy – What are the symptoms
Diabetic retinopathy has no warning signs in the early stages and vision may not be affected until the condition is severe. Symptoms can range from mild blurring initially to the loss of central vision.
Small spots in the vision or floaters may also indicate blood vessel leaks. Proliferative diabetic retinopathy can cause sudden severe vision loss from vitreous bleeding or tractional retinal detachment.
Because the disease is initially showing no symptoms and can be more easily treated in the earlier stages, it is important to have an eye examination annually, and immediately if you experience any of these symptoms. Late diagnosis and treatment can result in irreversible vision loss.
Diabetic Retinopathy – Prevention
Vision loss can be prevented with early detection. Annual eye checked by an ophthalmologist is very important.
Good diabetic control can slow down the development of diabetic retinopathy. Control of high blood pressure is also key in preventing the development and progression of diabetic retinopathy.
Other medical conditions such as high cholesterol, kidney disease and heart disease should be treated and kept under control. Giving up smoking, healthy diet and exercise regularly will maintain good diabetic control and reduce your risk of developing diabetic retinopathy.
Diabetic Retinopathy - Causes and Risk Factors
Who is at risk of developing diabetic retinopathy?
All diabetics are at risk of developing diabetic retinopathy. This is especially so if the diabetes is long-standing. After 20 years, most diabetics will develop this complication to some degree. Those who have poorly controlled diabetes are at higher risk of developing diabetic retinopathy earlier and at more severe stages.
People with diabetes should get a comprehensive dilated eye examination or screening at least once a year.
Diabetic Retinopathy - Diagnosis
Diabetic retinopathy is diagnosed with dilated retinal examination or retinal fundus photography.
Fundus photography can provide effective and efficient assessment of the diabetic retinopathy status in most patients.
If there are any abnormalities in the photography, you will be referred to your ophthalmologist for further assessment and management.
Diabetic Retinopathy - Treatments
Laser treatment procedure called laser photocoagulation can be performed to seal or destroy growing or leaking blood vessels in the retina.In general, each eye requires two to three sessions of laser treatment to be completed. adequately.
Anti VEGF injections are very good for patients with loss of central vision due to diabetic macular oedema, intravitreal injections of medication into the centre of the eye can reduce the macular swelling and improve vision.
Medications injected into the eye for diabetic macular oedema include Anti-Vascular Endothelial Growth Factor (VEGF) drugs such as Avastin, Accentrix and Eylea, as well as steroids.
Often, multiple injections at intervals of one month or longer are required to resolve the swelling. Repeated injections at longer intervals may also be required to maintain the visual improvement.
In some people with diabetic retinopathy, the abnormal blood vessels in the retina may also result in massive bleeding into the centre of the eye (vitreous haemorrhage), causing sudden severe loss of vision.
Vitrectomy surgery can be used to remove blood that is not clearing in the vitreous in the eye. Vitrectomy may also be required if there is a tractional retinal detachment. These cases, the visual outcomes are very guarded although some vision can still be regained or preserved by surgery.
Disclaimer – Above are just general information and patients are advised to see their Eye Doctors for professional treatment.
